Linda B Thompson, MD FACEP FAAEM
UAB School of Medicine
Department of Emergency Medicine
A 52-year-old Caucasian male who works as a construction worker presented to an Alabama emergency department (ED) with myalgias, fevers, rash, headache and neck stiffness that began four days prior. Two days into the illness, he noticed a necrotic lesion on his right flank which prompted him to visit his primary care doctor. He was given a steroid injection and discharged with a Medrol dose pack. For several hours after the steroid shot he felt improved. However, he presented to the ED when the underlying mild headache become more intense, the necrotic lesion became more painful, and a diffuse maculopapular erythematous rash developed. (Image 1) He admitted to removing 3 ticks off himself five days prior though none were attached to his skin or engorged. His blood pressure was 113/70 millimeters of mercury, heart rate was 63 beats per minutes, oxygen saturation was 98% at room air, and temperature was 97.7 degrees Fahrenheit. His laboratory tests showed a normal white blood cell count (WBC) 5.20 X 10 3/cells per cubic millimeter with 1% Bands, 10% Lymphocytes, 7% Monocytes, 6% Eosinophils and 5% Atypical Lymphocytes. The platelet count was slightly low at 129.0 X 103/ cubic millimeters. The Erythrocyte Sedimentation Rate (ESR) and the C-Reactive Protein (CRP) were elevated at 20 millimeters/hour and 26.04 milligrams/Liter, respectively. The following liver function tests were abnormally high: Total Bilirubin 1.7 milligrams/deciliter, Direct Bilirubin 0.4 milligrams/deciliter, Indirect Bilirubin 1.3 milligrams/deciliter, and Alkaline Phosphatase 143 units/Liter. The Alkaline Aminotransferase and Aspartate Aminotransferase were within normal limits, 56 units/liter and 37 unites/Liter respectively. The cerebral spinal fluid (CSF) glucose was low at 31 milligrams/deciliter and CSF protein was high at 93 milligrams/deciliter. The CSF WBC count was 1 cell/cubic millimeter and there were 0 CSF Red blood cells (RBCs) per cubic millimeters. A computed tomography (CT) of his head was normal. This patient was given IV Rocephin and oral Doxycycline for a presumptive tick-borne illness versus febrile illness of undetermined etiology. He was admitted for definitive diagnosis and was confirmed to have Rickettsial Parkeri. He was discharged within 48 hours to finish an oral course of Doxycycline. He made a full and uncomplicated recovery.
Discussion:
Exanthems are generalized skin eruptions described as erythematous maculopapular rashes that may be associated with fever or other systemic symptoms, usually of infectious etiology.¹ The exact mechanisms that lead to the rash eruption are not certain but can include “direct damage to cells by pathogenic organisms, toxin production by these organisms, and the patient’s immune response.”¹ Healthcare providers in emergency departments and primary care clinics often are the first line health care providers to assess exanthems. The exact diagnosis of a specific illness with a skin eruption often requires lab analysis such as serology testing [polymerase chain reaction] or a skin biopsy. These tests can take days to process and are not conducive to providing timely results. This lack of rapidly available diagnostic testing leaves the healthcare provider to make presumptive diagnoses and ultimate treatment decisions based upon clinical presentations and visual rash assessments. There are many visual similarities between exanthems and distinguishing the specific etiology can be a diagnostic challenge given the wide range of possible etiologies and the ease of worldwide travel.
This case is one such example.
This patient presented with an exanthem and an eschar. (Image 1)
A literature search [PubMed, Google Scholar, Medscape, UpToDate] led to the recognition that eschars can occur with exanthems or in non-exanthem rashes or wounds. Given this, the initial differential for this case included disease processes of skin eruptions that have an eschar-like component: Rickettsial infections, African Tick Bite Fever, Cutaneous Anthrax, Scrub Typhus, and Brown Recluse Spider bites, Pyroderma Gangrenosum, Ecthyma Gangernosum, and the Vasculidities such as Cryoglobulinemia Vasculitis. Each of these disease processes can be associated with fever or other systemic symptoms; however, Rickettsial infections are the only illness that can involve an exanthem, a generalized erythematous maculopapular rash, and an eschar. The other disease processes are not associated with exanthems.
This author purposes that an exanthem with eschar eruption makes these infectious processes a specific exanthem subset and when recognized can narrow the differential diagnosis based upon visual assessment and lead to more effective treatment. This is a case of an exanthem with eschar, which turned out to be Rickettsia Parkeri. These limited exanthems with eschars can universally be treated with Doxycycline. This patient was treated as such and completely recovered.
Image 1
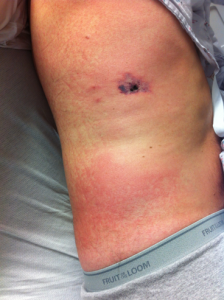
This image is reproduced with patient written permission.
References:
- Hartley H, Rasmussen J. Infectious Exanthems. Pediatrics in Review. April
1988. Vol 9;issue 10 - Paddock CD. Rickettsia parkeri as a Paradigm for Multiple Causes of Tick-Borne spotted fever in the Western Hemisphere. Annals of the New York Academy of Sciences. 1063:315-326 (2005)