Daniel M. Phillips, MS
Michael L. Sternberg, MD, FACEP, FAAEM
Department of Emergency Medicine,
University of South Alabama Health University Hospital
Mobile, Alabama
CASE DESCRIPTION
A 67-year-old male was transported to our level one trauma center after sustaining a thoracic crush injury at work. Pinned between hydraulic machinery for five minutes, the patient experienced a brief loss of consciousness, followed by severe chest pain. Physical examination was remarkable only for a respiratory rate of 22, agitation, palpable anterior chest wall tenderness, petechiae to the upper torso, neck, and face, and facial edema (Image 1). Eyelid ecchymoses, bilateral subconjunctival hemorrhaging and mild right ocular proptosis was also appreciated (Image 2). Radiographic investigation revealed right ocular exophthalmos with post septal intraconal hemorrhage, multiple bilateral rib and thoracic spinal fractures, and small bilateral pneumothoraces and hemothoraces. Admission and appropriate care provided, patient had an uneventful hospital course without long-term sequelae.
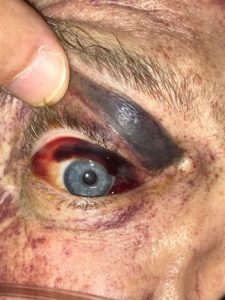 Image 1. Peri-orbital petechiae, eyelid ecchymosis, and orbital subconjunctival hemorrhage with chemosis (black arrows).
Image 1. Peri-orbital petechiae, eyelid ecchymosis, and orbital subconjunctival hemorrhage with chemosis (black arrows).
DISCUSSION
Traumatic asphyxia, also known as Olivier’s syndrome, Perthe’s syndrome, Masque Eccymotic, and compressive cyanosis, is a rare traumatic condition characterized by a triad of cervicofacial edema and cyanosis, subconjunctival hemorrhage, and facial, neck, and upper torso petechiae.[1,2] Most commonly seen in traffic accidents involving ejection with pinning underneath a motor vehicle or from heavy machinery, it is thought to be caused by simultaneous thoracoabdominal compression and a “fear response” (deep inspiration and closed glottis).[2,3] Elevations in central venous pressure transmit through the valve-less superior vena cava and innominate and jugular veins to produce cervicofacial cyanosis through capillary venous stasis and rupture.[2] The extent of damage is relative to both the amount of force and the duration of compression.[4] Associated injuries may include airway edema, visual blurring, diplopia, exophthalmos, hearing loss from eustachian tube edema and hemotympanum, and transient alterations in mental status, seizures, and hypoxic brain injury.[3,4] Cardiac damage is exceedingly rare and supportive care centered upon rapid reversal of cyanosis through oxygenation, intravenous hydration, and elevation of the head to lower intracranial pressure will usually result in a favorable outcome.[2,3,4]
LEARNING POINTS
Traumatic asphyxia classic triad: (1) cervicofacial and upper thorax petechiae, (2)
facial cyanosis and edema, and (3) subconjunctival hemorrhage.
Presentation to the Emergency Department with symptoms suggestive of traumatic asphyxia should prompt evaluation for associated injuries that may have been sustained from the crushing force to the chest.
Copyright permission has been obtained from the Department of Emergency Medicine, University of South Alabama Health University Hospital, Michael L. Sternberg, MD FACEP FAAEM.
REFERENCES
- Berkeley R, Bledsoe B, Markus T. Know the signs and symptoms of traumatic asphyxia. JEMS.2010;35(9):30,32,34.
- Richards CE, Wallis DN. Asphyxiation: a review. Trauma.2005;7:37-45.
- Sertaridou E, Papaioannou V, Kouliatsis G, et al. Traumatic asphyxia due to blunt chest trauma: a case report and literature review. J Med Case Rep. 2012;6:257.
- Gulbahar G, Kaplan T, Gundogdu A, et al. A rare and serious syndrome that requires attention in emergency service: traumatic asphyxia. Case Rep Emerg Med. 2015;2015:359814.